The Striking Difference in Neonatal Care Across the World
By Aimee Vaughn, MSN RNC-NIC, MGUH NICU QI and Patient Safety Coordinator, NANN Emerging Leader
NANN Footprints: Stories from the NICU January 2020
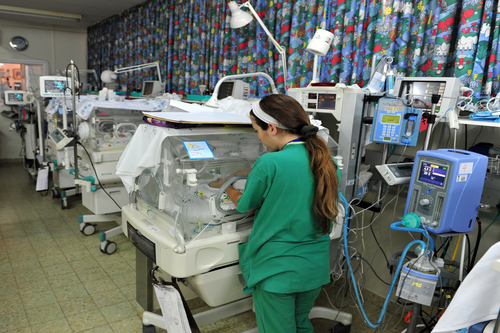 Consider the following stories of infants born with birth asphyxia and the care that they received….
Consider the following stories of infants born with birth asphyxia and the care that they received….
United States: The shift starts like many others. I am as assigned Delivery Room and Transport nurse. I begin taking care of my patients and completing my tasks, when we get a transport call.
Ghana: Meanwhile, in Ghana, the midwife shows up to the house of a family delivering their second child. The mother is in active labor.
United States: I pack up the transport bag, the transporter and prepare to leave.
Ghana: The midwife delivers the infant, who experiences birth asphyxia.
United States: My NICU transport team and I fly in the helicopter to get an infant that may need whole-body cooling. We arrive at the hospital when the infant is only one hour old.
Ghana: The midwife uses her knowledge of Helping Babies Breathe to resuscitate the infant.
United States: We stabilize the baby and place umbilical lines before returning to our hospital via helicopter. This is a sick baby, and we are happy the weather was cooperating enough to fly, rather than travel by ambulance. We arrive back at the hospital and start the whole-body cooling, video EEG, head ultrasound, continuous monitoring, dopamine, ventilation, UVC and UAC fluids within four hours of the baby being born.
Ghana: The midwife recognizes this baby needs advanced care and immediately gets a taxi. She travels in the taxi, alone, while using her knowledge of Helping Babies Breathe to continue to resuscitate the infant in the back of the taxi. It takes about four hours to arrive at the hospital. They do not do whole body cooling at that hospital. The infant is stabilized and cared for to the best of their ability. When the parents are able to care for the baby at home, the baby is discharged.
United States: Once the infant recovers from whole-body cooling, takes full feeds, and meets all necessary milestones we prepare the infant for discharge. The infant receives an MRI. The parents are educated on care of the infant for home. The infant is discharged to the parents with all necessary medications and follow-up appointments to ensure the infant will continue to have the best possible outcome.
These scenarios are real and demonstrate the difference in care across the world. I heard of the case in Ghana at a distance learning session for which I teach twice a month along with a physician at my U.S. based hospital. Eleven hospitals in Ghana participate in these sessions and at each one, a hospital presents a case based on the topic of the day. Based on the information provided in these case presentations, we improve and structure our education to meet their needs and consider their resources.
This particular case stuck with me. It was presented the day after I went on the transport for the infant described in the first scenario. I remember being annoyed that day because it took us longer than I wanted to get lines. I left that teaching session reminded of my privilege and all the resources we have here.
I get to live in a world that has made so many medical advances that there are treatments for infants with birth asphyxia. I get to live in a country where hospitals can transfer infants quickly to provide these treatments. I get to work at a hospital that provides these treatments. I am privileged to be a trained nurse who transports these sick babies back to my hospital.
Interested in sharing your Stories from the NICU? Contact Molly Anderson at This email address is being protected from spambots. You need JavaScript enabled to view it..
